‘Doing the best you can for your athletes’
Jamie Carlson has seen athletes come back from some remarkable injuries. “You hate to sell the human spirit short,” he said.
Carlson started at Wilfrid Laurier University as a certified athletic therapist nearly twenty years ago. Throughout his tenure, he has seen university athletes at the amateur level, the professional level and the international level get hurt with acute and chronic injuries.
And it always comes down to helping the athletes reach their full potential without succumbing to injury.
“It’s doing the best you can for your athletes,” Carlson said. “It’s a fine line between doing what’s best for them and kind of still allowing them to compete. My philosophy’s always been kind of if someone gets hurt, can I fix them by the time they have to play again? Or can we get them to play again?”
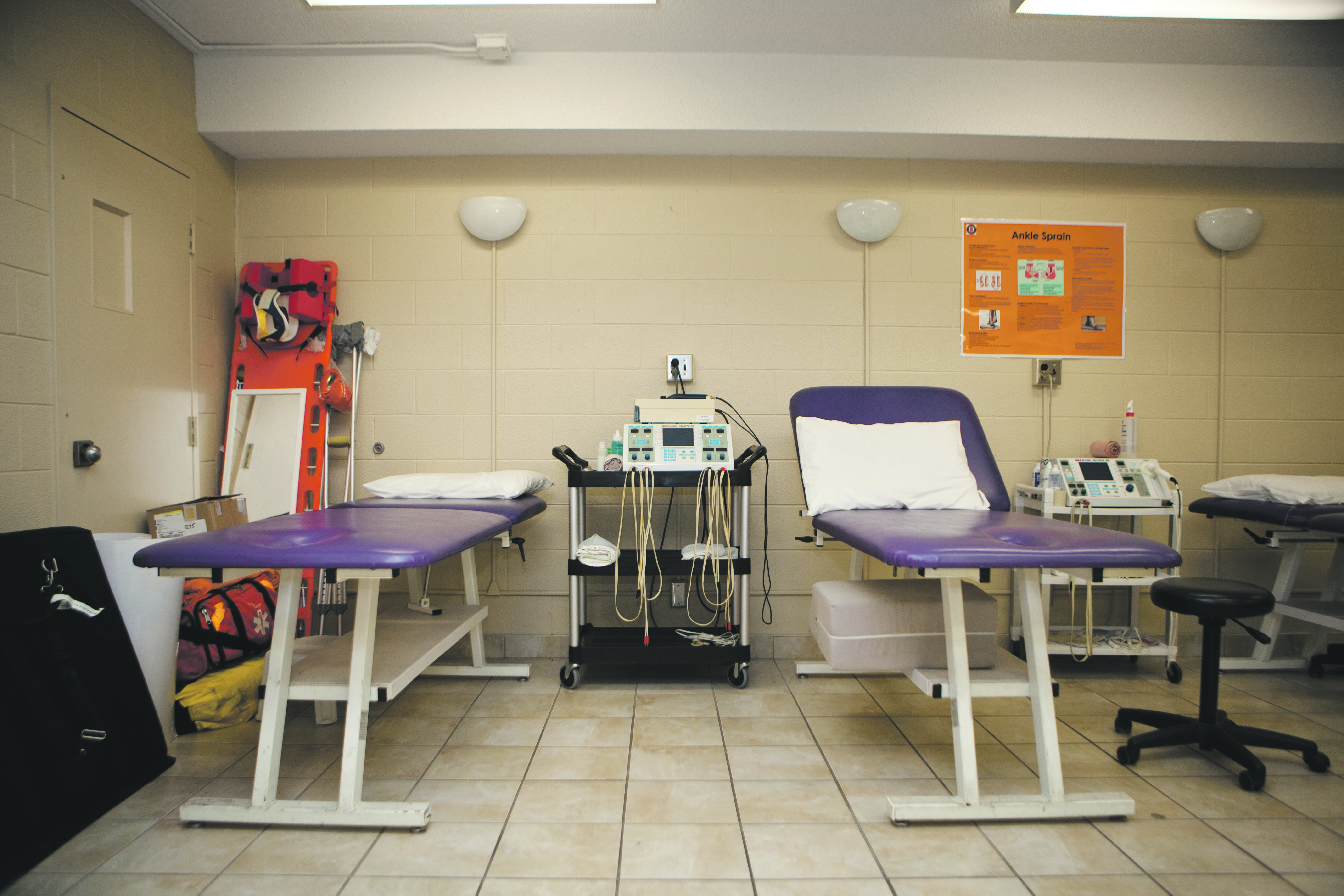
Athletic therapy focuses on the prevention and immediate care of injuries. Contrary to physiotherapy, athletic therapy centres primarily on the athlete and emergency care at the time of the injury.
According to Teresa Hussey, another certified athletic therapist at WLU and Sideline Therapy Clinic in Waterloo, there are two aspects to athletic therapy.
“There’s the clinical side, and then there’s the field side,” Hussey explained. “The clinical side would be very typical to your physiotherapy clinics. We do assessment, rehab, taking care of injuries, all of those types of things in a general clinical setting.
“The other side is the field side. So that’s all the on-field emergences, we do all the first aid, all the pre-game taping, post-game whatever needs to be done, but you’re there mainly for all of the emerg[ency] stuff.”
Athlete therapy is, mainly, total athlete care. The therapist can take care of anything from a minor ankle sprain during a soccer game to a major hip injury in a football game. The therapist must be ready to handle the injury on the field immediately.
“We’re a mish-mash of a trainer, ambulance attendant, physiologist, nutritionist; we’re all kind of packaged up into one ball,” Carlson said.
Because of the various natures of athletic injuries, protocol can change from case to case, depending on whether the injury is acute or chronic. However, there is a main process every athletic therapist follows when they are called onto the field, court or ice.
“It’s like anything. It’s a step-wise approach,” Carlson said. “You need to figure out exactly what you’re dealing with and figure out what the cause of the problem was.”
“When you’re treating someone on the field, [you are] kind of taking a quick history, doing a quick observation [and] special testing. That’s kind of what we consider our ‘quickie on field’ assessment,” Hussey continued.
After finishing the quick assessment, the therapist must decide whether the athlete can be taken off the field, and if so, how quickly and how safely.
As part of protocol, according to Carlson, the first 72 hours is inflammation control of the injury. Afterwards, the therapist progressively moves through tissue regeneration and reconditioning, then the question of returning to sport.
The difference in the process comes when dealing with acute or chronic injuries. Acute injuries are one-time injuries, and chronic injuries are persisting for a long time or constantly recurring. Both Hussey and Carlson stressed that while acute injuries follow a very basic rehabilitation depending on the nature of the injury, chronic injuries can be a lot more difficult to deal with.
“These cases, they’re a lot more complicated from the clinical side,” Hussey said. “You have to look at a lot more things from the whole body. So that’s when you start looking at what’s going on in the hips, is there a problem in the back or a problem in the knees or something that’s contributing to why they keep doing it. Which is sometimes easier said than done.”
To add to the factors, injuries can vary depending on the sport, and even the position. Hussey, who deals only with football, can see a variety of injuries during a game depending on which player gets hurt in which position.
“If you have soccer, generally soccer people all [have] the same structure,” she said. “But if you have an o-line, then you have a receiver or a quarterback, we’re talking two completely different things. So you can break it down, to each individual position almost has things that they are more likely to have happen to them. And that would be how you break it down because it’s such a different sport.“
The position, or sport, can evidently affect the return-to-play decision as well.
“When they’re coming back from injury, you need to know [everything],” Hussey said. “My o-line man doesn’t need to sprint more than five yards. So his perimeter for going back is going to be way different than a receiver who has to be able to spring 40 yards down the field.”
“You have to root around until you find out what all of the causes are,” Carlson said.
During their tenures as athletic therapists, Carlson and Hussey, alongside Jen Childs, who is also a certified athletic therapist* for WLU, have experienced very rare and traumatic injuries, including dislocated hips, serious concussions and possible spinal injuries. But despite the severity of the crazy occurrences in their jobs, both Carlson and Hussey dedicate themselves to maximizing the athlete’s performance without burden from an injury.
“At that time it doesn’t matter whose team is whose, we’ve got a kid that you don’t know if he’s going to walk or what’s going to happen,” Hussey said. “It’s a very rewarding job.”
* Editor’s note: This article has been changed since its original publication. *


